- Home
- Our Doctors
- Our Offices
- New Patients
- Patient Education
- Blog
- Contact Us
- Patient Portal Help
- Product Center

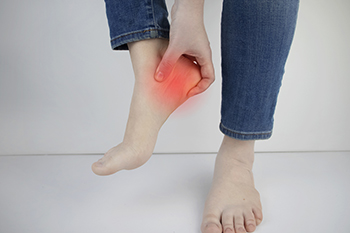
Tendons are fibrous tissues that connect muscles with bone. The Achilles tendon is the largest tendon in the body. It connects the calf muscles at the back of the leg with the heel, and facilitates movements such as jumping, running, and walking.
Because the Achilles tendon is engaged so frequently and bears a great deal of pressure and stress throughout the day, it can become injured. Achilles tendon injuries cause the tissue to become irritated, inflamed, and swollen. Pain can come on gradually or be immediate, and will vary from mild to severe depending upon the injury. Where the pain occurs will vary as well, from just above the heel up through the back of the leg. There may also be stiffness in the tendon.
Achilles tendon injuries can often be caused by repetitive stress. They may also occur while running, playing tennis, gymnastics, football, basketball, dancing, soccer, baseball or other sports that require speeding up, slowing down, or pivoting quickly. Wearing high heels, falling from an elevation, stepping in a hole, having flat feet, bone spurs, tight leg muscles or tendons, wearing improper athletic shoes, exercising on uneven surfaces, or starting a new type of exercise can also cause Achilles tendon injuries.
The two most common Achilles tendon injuries are tendonitis and ruptures. Tendonitis causes painful inflammation and can occur in different parts of the tendon. Non-insertional Achilles tendonitis occurs when the fibers in middle of the tendon begin to break down, thicken, and swell. This condition typically affects younger, more active adults. Insertional Achilles tendonitis occurs where the tendon inserts into the heel bone. It is common for bone spurs to form with this type of injury. This condition can affect people of any age and level of activity.
Achilles tendon ruptures are a tear in the tendon. These breaks may be partial or complete. There may be an audible popping noise at the moment of injury and the pain will be sudden and severe.
An Achilles tendon injury can be diagnosed by your podiatrist after they examine you, check your range of motion, and possibly perform a calf squeeze test or review an X-ray or MRI. Depending on the type and severity of your injury, your podiatrist may treat your condition with rest/ice/compression/elevation (RICE), nonsteroidal anti-inflammatory medications, heel lifts, and stretching and strengthening exercises. If you have torn your Achilles tendon, treatment may include physical therapy, ultrasound, shockwave therapy, or possibly even surgery.

A foot bath offers a myriad of health benefits that can enhance your overall well being. This ancient practice of immersing your feet in warm water has gained popularity in modern times. Foot baths have direct benefits for your feet. They soften and exfoliate the skin, preventing development of thick calluses. They also discourage bacterial buildup under toenails, cuts, and blisters, reducing the risk of infection. This is why pedicures often include a foot bath. Foot baths also aid in detoxification in the body and are beneficial for various medical conditions. Incorporating Epsom salt into your foot baths can help to manage muscle cramps, boost blood circulation, and reduce inflammation. Additionally, foot baths can also help to treat fungal infections, remove splinters, and provide foot pain relief. Essential oil foot baths add aroma therapeutic benefits to your soak. This can be beneficial in smoothing and moisturizing your skin, easing tired muscles, and reducing stiff joints. Soaking your feet in apple cider vinegar offers various health benefits as well, including treating fungal infections, soothing sore feet, and healing dry skin. If you would like to learn more about the benefits of foot therapy, such as foot baths, it is suggested that you make an appointment with a podiatrist.
Foot therapy is often necessary for those recovering from either foot deformities or foot injuries. If you have concerns regarding therapy, consult with one of our podiatrists from Foot & Ankle Institue. Our doctors can provide the care you need to keep you pain-free and on your feet.
Most Common Injuries
People who are active or athletes are prone to a variety of injuries. Therefore, it is often important to take part in physical therapy in order to quickly get back on the right track.
What to Do When Injured
Physical Therapy – This specialized treatment will focus on the affected area, speeding up recovery and the overall healing process. It is a proven method that has helped millions of people return from any injury.
During physical therapy you will undergo regimented training to get back into full form. Training is often very difficult, especially at first when the foot feels weak. Physical therapy often involves:
Basic stretching and twisting exercises – getting the feet’s mobility and flexibility up.
Massaging – the therapist will massage the injured area in order to activate the muscles and relax them.
Strengthening Exercises – this allows the muscles in the affected area to regain their full strength, a vital step towards full recovery.
If you have any questions please feel free to contact one of our offices located in St. George, Hurricane, and Cedar City, UT and Mesquite, NV . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Foot Therapy for Sports Injuries
Athletes are used to engaging in high-intensity workouts. Consequently, athletes are at an increased risk for enduring foot or ankle injuries. The most common way to treat these types of injuries is the RICE method (Rest, Ice, Compression, and Elevation). However, braces and casts may be required in some cases. If you are suffering from any of these injuries, it is best that you seek help from your podiatrist right away.
Achilles Tendinitis
Achilles tendinitis is a type of overuse injury of the Achilles tendon, which is the tendon connecting the calf muscles to the heel. This type of injury commonly occurs in runners who increase the intensity of their workouts. Symptoms for this condition start off as a mild ache in the back leg or above the heel. Some people experience tenderness around the area in the morning, however this feeling tends to improve over time. If you suspect you have Achilles tendinitis, you doctor may order an x-ray to show whether your Achilles tendon has calcified. Common treatment options for this condition include rest, ice, exercise, and non-steroidal anti-inflammatory medication.
Plantar Fasciitis
Plantar Fasciitis is a condition that is commonly found in women. It is a painful condition that occurs when the bands of tissue that connect the heel to the toes become inflamed. Symptoms for plantar fasciitis are heel pain that worsens in the morning and improves throughout the day with activity. Your podiatrist will diagnose plantar fasciitis by checking for tender areas on your foot. In rare cases, an x-ray may be required for a more thorough examination. There are various treatment options that may be used to help someone with this ailment. Depending on the specific case, some of these options include: physical therapy, shockwave therapy, and in rare cases, surgery.
Stress Fractures
Stress fractures are tiny cracks in the bone that occur due to repetitive force. These fractures are typically the result of overuse injuries such as repeatedly running and jumping. Symptoms of a stress fracture include pain when exercising, tenderness, and mild swelling. To diagnose a stress fracture, your doctor will likely ask you a series of questions about your overall health and the activities you are involved in. Next, an x-ray will likely be performed to check for the fracture. In some cases, fractures don’t appear on x-rays until weeks afterward. In these cases, an MRI or a bone scan may be required. Typical stress fractures may be treated by resting the area and taking a break from highly intense activities.
Ankle Sprain
Ankle sprains occur when the ligaments that support the ankle are stretched far beyond their limits. These injuries occur when you roll, twist, or turn your ankle in an awkward way. Ligaments are essential in helping us move around because they are responsible for stabilizing the joints. Usually, sprained ankles occur due to ligaments on the outer part of the ankle becoming stretched. Symptoms of ankle sprains are swelling, bruising, instability of the ankle, and restricted range of motion. Normally, when people sprain their ankle, they will hear a popping sound during the injury. Depending on the severity, ankle sprains are graded based on how much damage has occurred to the ligaments. Grade 1 is mild, grade 2 is moderate, and grade 3 is severe.

Flat feet, medically known as pes planus, is a common condition where the arches of the feet appear flattened, causing the entire sole to make contact with the ground. Flat feet can be a result of genetics, injury, or muscle weakness. While many individuals with flat feet may not experience pain, others can suffer from discomfort and fatigue, especially during prolonged periods of standing or physical activity. Fortunately, there are steps that can be taken which may help to alleviate flat feet pain. This can begin by wearing supportive shoes with arch support and cushioning. Custom orthotic inserts can also provide additional support and comfort. Stretching exercises for the Achilles tendon and calf muscles can help improve foot flexibility. Additionally, performing strengthening exercises for the foot and ankle muscles can enhance arch support. By addressing flat feet and taking proactive measures, you can find relief from discomfort and improve your overall foot health. If you have flat feet, it is suggested that you visit a podiatrist who can guide you toward additional relief options.
Flatfoot is a condition many people suffer from. If you have flat feet, contact one of our podiatrists from Foot & Ankle Institue. Our doctors will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact one of our offices located in St. George, Hurricane, and Cedar City, UT and Mesquite, NV . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot is classified as having the entire sole of the foot in contact or near contact to the ground while standing. The disorder is also known as fallen arches, because those affected have no arch in their feet. Flexible flatfoot and rigid flatfoot are the two types of flatfoot.
A person has flexible flatfoot if when sitting or standing on their toes, they have an arch that disappears when they stand with the entire foot on the ground. Flexible flatfoot may also be called “pediatric flatfoot” because the condition first appears in childhood. It is common among infants because the arch does not develop until the age of 5 or 6 years. Rigid flatfoot is not as common in children as it is with adults. This type of flatfoot is developed due to the weakening of tibialis posterior muscle tendon, a major supporting structure of the foot arch. Development of this deformity is progressive and shows early signs of pain and swelling that begins at the inside arch of the foot and moves to the outside of the foot below the ankle. More severe cases can possibly lead to arthritis of the foot and ankle joints.
Although most cases of flatfoot involve people born with the condition, some less common causes are obesity, diabetes, pregnancy, and osteoporosis. In some cases, flatfoot may come with no symptoms at all and does not require any type of treatment. With other cases though, symptoms may include pain in the shin, knee, hips and lower back. If a person with flatfeet experiences such symptoms, a health care provider may suggest using orthotic devices or arch supports, which may reduce the pain. Wearing supportive shoes can also prove more comfortable with flatfeet and staying away from shoes with little support such as sandals. Other methods to relieve pain also include stretching the Achilles tendon properly and using proper form when doing any physical activity. In addition, losing weight can reduce the stress on your feet and reduce the pain.
Plantar fasciitis, a prevalent foot condition, can cast a shadow on even the most active lifestyles. It occurs when the plantar fascia, which is defined as the ligament connecting the heel bone to the toes, becomes inflamed or strained. There are various reasons for plantar fasciitis, often stemming from repetitive stress, poor footwear choices, obesity, or abnormal foot structures, such as flat feet. Symptoms encompass sharp heel pain, especially during the first steps in the morning or after periods of inactivity. As painful as this condition can be, there are various options that can be implemented. Treatment methods can range from rest, and taking over-the-counter pain medications to targeted exercises that stretch and strengthen the plantar fascia. In more severe cases, podiatrists may recommend custom orthotics or corticosteroid injections. With proper care and attention, managing plantar fasciitis can help individuals step back into a life unhindered by foot discomfort. If you have developed plantar fasciitis, it is strongly suggested that you are under the care of a podiatrist who can determine what the best course of treatment is for you.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from Foot & Ankle Institue. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact one of our offices located in St. George, Hurricane, and Cedar City, UT and Mesquite, NV . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.

A plantar fibroma is a benign and non-cancerous growth that forms on the thick band of tissue on the bottom of the foot known as the plantar fascia. These fibromas typically develop slowly and are often painless, but they can cause discomfort or pain when pressure is applied. The exact cause of plantar fibromas is not fully understood, but they are thought to be related to genetic factors or trauma to the foot. Treatment for plantar fibromas depends on their size and the level of discomfort they cause. Non-surgical options such as orthotics, or corticosteroid injections may help to alleviate symptoms. However, in more severe cases, surgical removal of the fibroma may be necessary to relieve pain and restore foot function. Early diagnosis and intervention are essential to effectively manage plantar fibromas and prevent complications. If you have a growth on the bottom of your foot, it is suggested that you confer with a podiatrist who can diagnose a plantar fibroma, and offer treatment options that are correct for you.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact one of our podiatrists of Foot & Ankle Institue. Our doctors can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions please feel free to contact one of our offices located in St. George, Hurricane, and Cedar City, UT and Mesquite, NV . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
A plantar fibroma is a knot in the arch of the foot. It can cause pain when repeated pressure is applied by walking barefoot or wearing tight shoes. While plantar fibromas can appear in anyone, men who are middle-aged or older are said to be more susceptible. The main symptom of a plantar fibroma is a firm lump on the arch of the foot. If there is pain, it can be intensified by putting pressure on the nodule. The lump can stay one size or grow larger. You may have one or more fibromas in the feet and there tends to be a high incidence of recurring plantar fibromas. Generally, a plantar fibroma can be treated without surgery. Treatment might include steroid injections to help shrink the lump, orthotics to help redistribute weight away from the nodule, plantar fascia stretching, or physical therapy to help use anti-inflammatory medication on the lump. If a lump grows larger or more painful, a podiatrist can be consulted to confirm the diagnosis. The doctor will palpate the lump and this may cause pain that can be felt all the way to the toes. An X-ray, MRI, or biopsy might be done if further evaluation is necessary. A lump in the arch of the foot might be something other than a plantar fibroma, such as cysts, nerve or fatty tumors, swollen tendons, or an infection in the foot. It is important to see a podiatrist for proper diagnosis and treatment of plantar fibromas.
Having issues or need help with your portal?
Click here for Instructional Videos